I would guess the man was in his mid-forties.
Seated at a small two top in Starbucks with a woman maybe about his age, I was nearby and happened to hear some of their conversation.
Now, I don’t generally eavesdrop and but I could not NOT listen.
He was talking talking about knee pain. Apparently he’d had it for a while. He sounded frustrated. And from what I heard, he felt that his options were few.
“The doctor said I would just have to live with it and that I should just quit running and stuff.”
I was told that years ago when I had knee surgery – that I would never run again. Sometimes, that’s true. But many times, it’s not.
The discussion reminded me of an article just a couple of years ago in the LA Times on the same subject – that there was no easy fix for painful knees.
Well, of course that’s true.
There is no easy fix for knees that hurt, that may be swollen, have weak cartilage, and belong to someone who wants to stay active.
According to the article, “Active people in their 40s and 50s are challenging doctors to provide treatments that not only keep them walking but keep them running and jumping as well.”
And then later, “….scientists at Exponent Inc., a scientific consulting firm, projected that the demand for replacement knee joints would more than sextuple by 2030, with 3.48 million people in need of a new knee.”
Dr. Andrew Spitzer, the director of the joint replacement program at the Cedars-Sinai Orthopaedic Center in Los Angeles, believes that one of the reasons for the rise in knee pain and demand for surgery is that people are “keeping fit” but that this activity is creating too much physical stress and leads to wear and tear of the joint.
I don’t think you can call yourself fit if, when you go for a run, your knee swells, you limp for three days, then hurt for ten more days and eat Advil like sweet tarts. I think you may be fit in certain parts of your body. You may have enough flexibility but your your joints aren’t fit.
They’re giving you fits.
How A Joint Heals
The strategy I used to help rebuild my ability to run is based on the science of mechanobiology.
Mechanobiology is the study of how mechanical forces generated within or imposed upon living tissues affect the physiology and structure of that tissue. So, in other words, how do various types of movement impact the healing of injured or painful tissue?
The problem is, in most cases, not that you’re not fit but that your joint is not fit.
Joint fitness depends on something called “mechanotransduction” – the process the body uses to convert force into cellular responses.
Okay. I know. All of that has a high geek factor but it’s important.
The best known application of mechanotransduction is bone healing. When you break a bone, the bone heals from the application of force. The force alters cell response. It tells the cells what to do. Too much force, too soon, and the bone heals slowly or sometimes not at all. The same goes for too little force for too long. Incomplete bone healing.
When it comes to a joint, and in particular the joint cartilage, clinicians and the general public struggle with the idea that the same principle applied to bone could apply to cartilage even though there’s evidence suggesting that it does.1, 2
So, instead people try to increase their quadriceps strength. The idea is that by having stronger quads, you’ll “protect” the joint.
What happens though is that the level of force or resistance you need to strengthen the leg exceeds the joint’s fitness level and you hurt. You never really get as strong as you need, because the joint simply can’t take the load.
Cartilage has no blood supply so the only way it gets the nutrients it needs is from the underlying bone and the synovial fluid within the joint. The joint needs a lot of movement at a low level of force. And it also needs to be nudged not pushed. Easy does it wins more often than “no pain no gain”.
Tips On Improving Joint Fitness
If you have an achy, painful knee, finding out what tissue or tissues are injured is very helpful (and my advice, avoid Dr, Google, Dr. Bing or Dr. Yahoo). But lets assume for now that the problem is weak cartilage – often found in Patellofemoral Syndrome, Osteoarthritis, Runner’s Knee Syndrome and other types of joint problems.
- Foot slides. You can use a paper plate for this. Sit in a comfortable chair, place your foot on the paper plate and slide your foot forward and back. The load with this drill is very low and so is the level of interest. I suggest reading a book, watching a movie or whatever you need to occupy your mind because otherwise, you won’t last long. The goal is thirty minutes per day (for any of the items in this list except “quad sets”). You can divide it into small chunks as needed but five to ten minutes per session seems to work well.
- Stationary cycling. Easy does it though. With an work output of 120 watts, you can easily exceed body weight force in the joint. Choose a low resistance and just take a nice easy spin rate. And books & movies are your friends again.
- The Restorator. This looks like a gimmick but it works pretty well for this application. It’s easier way to perform the cycling motion, takes up a small amount of space too.

- Total Trainer. This is my preference. Yes, it’s more money. Yes, it takes up more space but it gives you way more control over “nudging” your joint into higher levels of fitness. It works by using a percentage of gravity for the load. This then makes the loads specific to you. I’ve used this and like it. We also use this in our coaching studio. You find a pain free level of force – often down near the bottom of the rung ladder and perform squats, nice and easy, slowly, to a 90-degree knee angle. And again, you’re shooting for a high volume of reps so start out with 5-10 minutes and do 4-5 sessions a day. As your knee gets stronger, you can increase the angle.

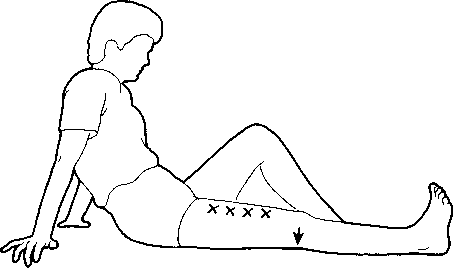
- Quad sets. The old standby often suggested as a way to “strength the quads” which of course it doesn’t do since your joint doesn’t move and there’s no additional load to make the muscles work harder. To do a quad set, you tighten the thigh muscles as tightly as you can and hold for five to ten seconds and then relax. The goal is 100 repetitions per day. For those of you who like to know why this helps you, quad sets have been shown to increase the molecular weight of synovial fluid which makes the fluid thicker or more viscous. ((Miyaguchi, M., A. Kobayashi, et al. (2003). “Biochemical change in joint fluid after isometric quadriceps exercise for patients with osteoarthritis of the knee.” Osteoarthritis Cartilage 11(4): 252-9.)) This then serves as an extra from or protection for your joint.
And, by the way, the LA Times article lists options for people with knee joint pain and one of them, and I’m going to quote this because it seems so bizarre is “…Pain killers and anti-inflammatories are a good option for early arthritis, Feeley says, “if they relieve your pain and allow you to stay active.”
Well, sometimes, yes, that’s what you must do to get through life. But, what most people do is eat a few Motrin or Advil and then go for a run or workout hoping the drug will keep from hurting or swelling or having a stiff achy knee the next day. That is not a good idea. What you’re doing is overloading a weak joint and delaying the inevitable – pain, stiffness, swelling (if you want the whole LA Times article, click here).
1. Roos, E. M. and L. Dahlberg (2005). “Positive effects of moderate exercise on glycosaminoglycan content in knee cartilage: a four-month, randomized, controlled trial in patients at risk of osteoarthritis.” Arthritis Rheum 52(11): 3507-14.
2. Roos, E. M. and L. Dahlberg (2004). “[Physical activity as medication against arthrosis–training has a positive effect on the cartilage].” Lakartidningen 101(25): 2178-81.



